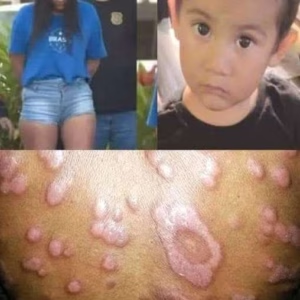
Shingles, scientifically known as herpes zoster, is a condition that often triggers concern and confusion, particularly because many people are unaware of its origins or why it manifests in those who appear to lead healthy lives. While it is a relatively common condition, especially as individuals age, understanding its mechanics is vital for acting promptly and preventing serious complications.
Shingles is directly linked to the varicella-zoster virus, the same pathogen responsible for chickenpox during childhood. A little-known fact is that once a case of chickenpox resolves, the virus does not leave the body. Instead, it remains dormant for years or even decades, hiding within the nervous system. Under specific conditions, such as a weakened immune system, the virus can reactivate. Factors that contribute to this reactivation include the natural aging process, prolonged stress, chronic illnesses, medical treatments that suppress immune function, or periods of intense physical and emotional strain. While more prevalent in adults over 50, it can nonetheless affect younger individuals.
The disease rarely appears without warning. Often, the initial symptoms are nonspecific and can be easily mistaken for other health issues. Patients may experience localized pain, burning, tingling, or skin hypersensitivity days before any visible rash emerges. These early warning signs make prompt diagnosis challenging if they are not carefully monitored. As the virus progresses, a localized rash typically develops on only one side of the body. This specific pattern occurs because the virus reactivates along a particular nerve pathway, restricting the lesions to a defined area rather than allowing them to spread throughout the body.
While the external rash is striking, medical professionals emphasize that the associated pain can be the most debilitating and persistent symptom. With appropriate medical treatment, most cases have a favorable outcome. Antiviral medications, when administered within the first 72 hours of symptom onset, can significantly shorten the duration of the illness and reduce the risk of complications. When diagnosis is delayed, however, patients risk developing postherpetic neuralgia—a form of chronic, persistent pain that can last for months or even years after the rash has cleared. This long-term pain often interferes with sleep, daily activities, and general emotional well-being, which is why doctors emphasize that patients should never minimize early signs and should seek medical advice immediately.
Regarding contagiousness, shingles is not contagious in the traditional sense. A person with shingles cannot directly transmit the condition to another person, but they can transmit the varicella-zoster virus to someone who has never had chickenpox or been vaccinated. In that case, the recipient would develop chickenpox rather than shingles. To be safe, it is recommended that those with an active rash avoid direct contact with newborns, pregnant women, and immunocompromised individuals.
In recent years, prevention strategies have become paramount. Vaccines are now available to reduce the risk of developing shingles and to lessen the severity of the illness should it occur. Health organizations strongly recommend these vaccines for older adults and those with specific risk factors.
Ultimately, shingles serves as a reminder that health is not merely the absence of visible illness. Maintaining a balanced immune system, managing stress, and staying attuned to the body’s subtle warning signals are essential. By understanding the origins of the virus and recognizing early indicators, individuals can take prompt action, sparing themselves from prolonged pain and unnecessary complications. Informed vigilance is the best defense against this silent, recurring threat.